For decades, the idea of taking insulin as a pill has been one of diabetes research’s most persistent goals. The problem has always been the same: insulin is easily broken down in the digestive tract, and the intestine does not naturally absorb it into the bloodstream.
Now, researchers at Kumamoto University report a peptide-based workaround that may make oral insulin more feasible. Their approach uses a small cyclic peptide called DNP, which appears to help insulin move through the small intestine instead of being destroyed before it can act.
Two ways to carry insulin across the gut
The team tested two delivery strategies. In one, they mixed a modified peptide, D-DNP-V, with zinc-stabilized insulin hexamers. In diabetic mouse models, this oral formulation lowered blood glucose rapidly and kept it controlled with once-daily dosing over three days.
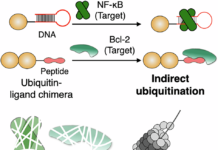
In the second strategy, the researchers used click chemistry to permanently attach the DNP peptide to insulin, creating a DNP-insulin conjugate. That version also produced strong glucose-lowering effects, supporting the idea that the peptide itself is doing the transport work across the intestinal barrier.
Lower doses may make oral insulin more realistic
One of the biggest barriers to oral insulin has been poor efficiency, which often forces developers to use extremely high doses. According to the study, the new platform achieved a pharmacological bioavailability of about 33% to 41% compared with subcutaneous injection. That is still not the same as an injection, but it is a major step toward practical oral dosing.
“Insulin injections remain a daily burden for many patients,” said Associate Professor Shingo Ito, who led the project. He added that the peptide platform may also be useful for long-acting insulin formulations and other injectable biologics.
What comes next
The work, published in Molecular Pharmaceutics, was performed in diabetic mice, so human use remains a future goal rather than a near-term reality. The researchers are now planning additional testing in larger animals and in systems that better mimic the human intestine.
Still, the study offers a compelling proof of concept: a small peptide may be able to solve one of medicine’s oldest drug-delivery problems and bring the long-promised insulin pill closer to patients.